Steps, calories ... blood? The wellness industry is coming for our sugar levels
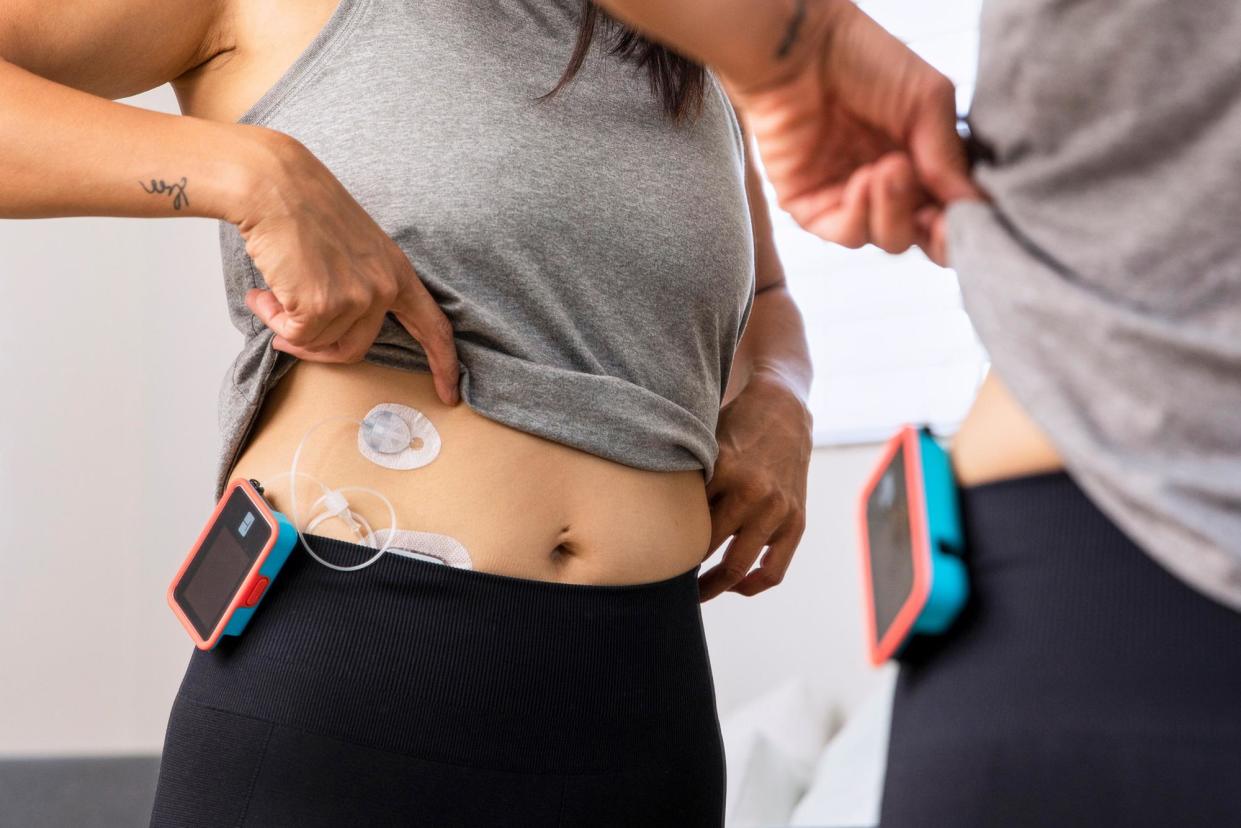
It’s easier than ever to monitor our step count, calorie intake and sleep cycles. Now the personal-data trend has come for blood sugar levels.
Biotech companies like Zoe, Signos and Nutrisense are marketing continuous glucose monitors, or CGMs – disposable devices with a tiny, needle-like sensor – to people without diabetes who want to know how their bodies process foods.
CGMs tout an edge in personal health optimization, but are these devices genuinely beneficial tools for understanding and improving health, or just the latest trend among the worried well?
Related: Are you always late? Here’s how to be on time
How do continuous glucose monitors work?
Rather than measure sugar levels in blood directly, as one might do with a finger-prick test, CGM devices measure sugar in the interstitial fluid around cells. As a result, their readings can lag behind real-time blood sugar levels by five to 20 minutes, which could be an issue for people with diabetes who need to respond to sudden shifts, but is typically less problematic for those without diabetes.
CGM companies typically offer subscription plans. For instance, a three-month subscription with Nutrisense is priced at $299 per month, whereas Signos offers a similar plan for $229. Subscribers receive two CGMs a month; these devices are affixed to the outer arm and secured with a waterproof bandage, remaining functional for 14 days. Alongside the hardware, users gain access to a companion app that illustrates their blood sugar levels fluctuating in near-real time. Some companies also provide personalized diet and exercise information designed to help users reach their health goals.
How do blood sugar levels relate to our health?
People with diabetes need to monitor their blood sugar levels because their bodies have trouble producing or using insulin, a hormone created by the pancreas that helps cells absorb sugar from the bloodstream. For people with diabetes, regulating blood sugar through a vigilant routine of diet, physical activity and insulin injections is crucial to minimizing the risk of severe complications, including heart disease, strokes, kidney failure and blindness.
CGM marketing often suggests that even if one does not have diabetes, and has relatively consistent blood sugar levels, further stabilizing those levels can enhance overall health and facilitate weight loss.
Related: Introducing Well Actually, the Guardian’s weekly wellness newsletter
Signos’s website urges: “Avoid glucose spikes as much as possible.”
“Your body needs to keep a tight rein on glucose. If the balance tips in either direction, it can be bad news,” reads a post on Zoe’s site.
While a glucose spike after a big dessert or a carbohydrate-heavy lunch may result in some immediate effects, like fatigue or difficulty concentrating, occasional spikes aren’t a cause for concern for most. However, it’s true that uncontrolled, frequent, high blood sugar spikes can cumulatively contribute to the development of insulin resistance in anyone. When blood sugar levels surge, the pancreas is forced to produce more insulin. Long periods – typically years – of consistent spikes can eventually impair our body’s ability to use insulin effectively and may also slow down insulin production. This can result in pre-diabetes, a reversible condition where blood sugar levels are elevated above normal. Without intervention, these recurring spikes can gradually lead to type two diabetes.
What’s the benefit of monitoring blood sugar for healthy people without diabetes?
A 2018 Stanford University study of healthy individuals using CGMs found that glucose dysregulation, characterized by excessively high glucose spikes, may be more common in healthy people without diabetes than previously thought. “We saw that some folks who think they’re healthy actually are misregulating glucose – sometimes at the same severity of people with diabetes – and they have no idea,” writes Michael Snyder, professor and chair of genetics at Stanford and senior author of the study. If your CGM reveals that your body has not been controlling your blood sugar very well, that information could be relevant to your health.
But doctors and scientists don’t all agree that CGMs can help make truly healthy individuals even healthier. Harvard Health’s Robert H Shmerling has written that there’s currently no impartial published research linking CGM use by people without diabetes to better health outcomes or weight loss, and that more research needs to be done to prove the value of these devices. Endocrinologists say that healthy people are unlikely to see significant changes in their blood sugar levels at all, because their bodies process sugar efficiently, making these monitors more useful for satisfying personal curiosity than meaningfully improving health.
Nonetheless, some may find that using a CGM to observe how conventional health knowledge applies to their bodies in real time is worthwhile. Watching your blood sugar rise after eating a slice of chocolate cake might be more impactful than reading about how cake affects your body, said the McGill University endocrinologist Kaberi Dasgupta. “Companies are using this self-monitoring to help people personally arrive at the conclusion that the literature has arrived at: physical activity and eating whole foods is good for our overall health,” she said.
Yet, for people without diabetes who tend to stay within a healthy range (usually under 140mg of sugar per decilitre of blood, post-meal), this kind of information could amount to splitting hairs. “As long as you keep your sugars under a certain threshold for the most part, you don’t need to worry about the variations within it,” said Nitai Gelber, an Ontario-based family physician. “Your blood sugar can go up to [140mg/dl] after meals without cause for worry. There’s no need to try and flatten your levels further when your body is already doing an excellent job.”
Can CGMs help people with pre-diabetes or the insulin-resistant?
Toronto resident Justin Richard, 52, posts TikTok content about using a CGM to monitor his body’s response to different foods. Richard said that throughout his 40s, he found himself losing energy and feeling generally unwell, with a tingling sensation in his hands and feet. Knowing he had a family history of diabetes, and somewhat of a “junk food addiction”, he went to his doctor, only to be told nothing was wrong. Nonetheless, Richard suspected he was insulin-resistant, because the condition results in neuropathic symptoms like tingling.
“Year after year, I was just declining,” Richard said. A 2019 study found that meaningful physician knowledge gaps in pre-diabetes diagnosis and treatment plans can mean some patients slip through the cracks. Pre-diabetes can also be a symptom-free “silent” condition; 80% of people with pre-diabetes don’t know they have it.
Richard started using a CGM more than a year ago to monitor his blood sugar so he won’t “automatically go into type two diabetes” due to lack of medical intervention, which happened to his mother, he said. He has not yet received a pre-diabetes diagnosis from a doctor. He’s found he feels better and more energetic when he’s able to keep his blood sugar within a healthy range.
“Awareness keeps me in check,” he says. “When I eat something and my blood sugar goes up, it’s a reminder that: ‘Hey, you really could be causing damage to yourself by eating these types of foods over the long haul.’ Diabetes doesn’t happen overnight. It’s decades in the making.”
Are there downsides to using a CGM if you don’t have diabetes?
CGMs are expensive, and there’s a possibility they may not give users much dietary insight they couldn’t find elsewhere free of charge.
Dasgupta warns that CGM users who are not working with a doctor to interpret their data may overlook how other factors like stress and sleep quality affect their blood sugar.
Related: ‘The world became so loud’: what it’s like to suddenly lose your hearing
Moreover, using CGMs may encourage users to over-focus on balancing their blood sugar. “When you’re doing that kind of self-testing, there is definitely a risk that you become obsessed with it,” said Dasgupta. For instance, a user may worry about the normal blood sugar fluctuations following any meal, or fixate on how their body reacts to certain foods, even within a healthy range.
While it’s not a downside per se, the rise in CGM use among people without diabetes is unlikely to meaningfully stem surging diabetes rates. Researchers believe that just under half a billion people are living with diabetes worldwide, and project that number will increase 25% by 2030 and 51% by 2045. Diabetes is most prevalent in higher-income countries, but in those countries, people with lower incomes experience higher rates of the disease, which could mean CGMs may be inaccessible to those who need them most.


