Pancreatic cancer: Symptoms, causes and treatment
As one of the world’s leading experts in pancreatic cancer, Prof Andrew Biankin is all too familiar with the aura of dread which surrounds the disease.
“There’s something about the cancer that makes it inherently aggressive,” says Prof Biankin who directs a research centre at the University of Glasgow. “It’s viewed by many drug developers as the graveyard of therapeutics because it’s very difficult to treat.”
There are more than 9,000 new cases of pancreatic cancer in the UK each year, and while the prognosis is typically grim, researchers are hopeful that novel diagnosis and drug technologies can provide more hope for patients in years to come.
But like all cancers, pancreatic cancer comes in many different forms. So what are they, and how are cancer experts working to detect and treat them more effectively?
Jump to:
What is pancreatic cancer?
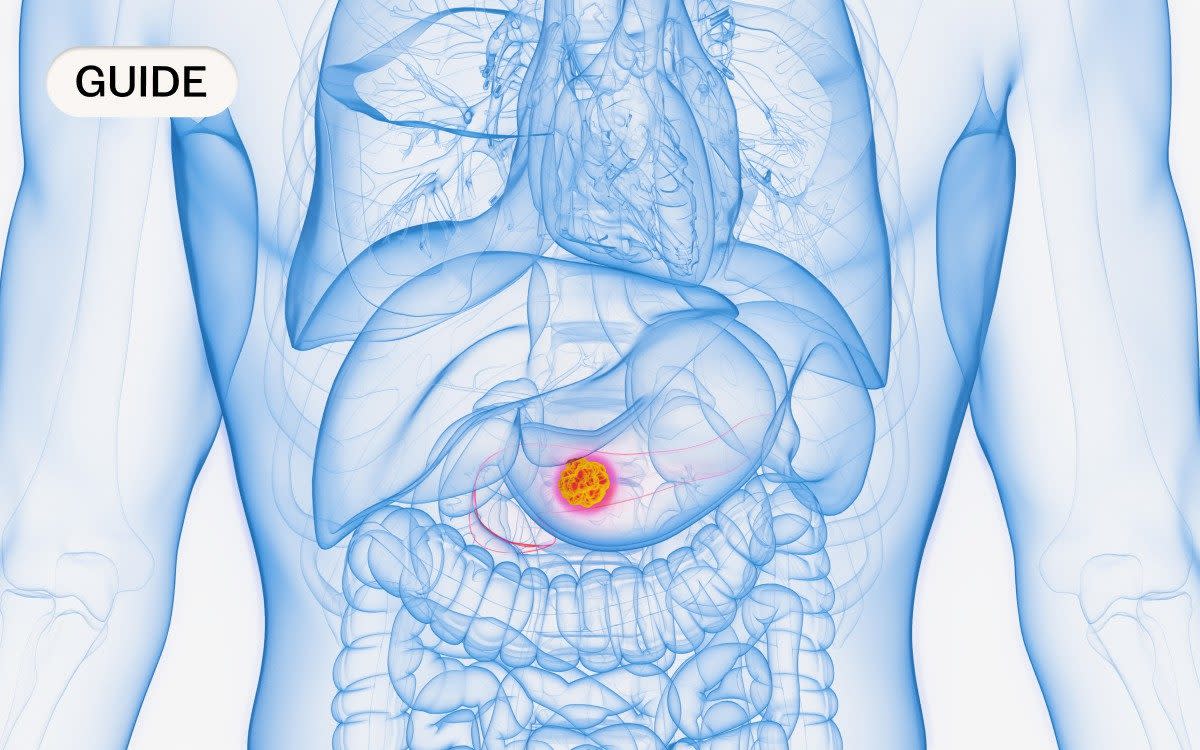
Quite simply, pancreatic cancer is caused by the abnormal and uncontrolled growth of the cells in the pancreas. However, the disease is fuelled by far more than just the cancer cells themselves, which explains its resistance to many common treatments.
“Within pancreatic tumours, there is a significant presence of cells called cancer-associated fibroblasts,” says Anguraj Sadanandam of The Institute of Cancer Research in London. “The build-up of these fibroblasts can cause the tumours to become dense and hard, making it difficult for drugs to penetrate them effectively. Additionally, pancreatic tumours have fewer active immune cells than other cancers, making them less susceptible to destruction by the body’s immune system.”
What are the different types?
Around 95 per cent of pancreatic cancers are known as exocrine pancreatic cancer, which means that they develop from the cells found in the exocrine gland and ducts of the pancreas. Pancreatic cancers overwhelmingly begin in the lining of the ducts within the organ, with adenocarcinoma being the most common form of exocrine pancreatic cancer.
According to Ricky Bhogal, a consultant at the Royal Marsden Hospital, adenocarcinomas in the pancreas are aggressive and difficult to treat because these tumours tend to attach themselves around the major blood vessels which run through the abdomen. “Any tumour, even if it’s small, has a high tendency to involve these blood vessels,” he says. “The operation becomes much more tricky and technically difficult to do because however we do it, those blood vessels have to remain in place at the end of the procedure.”
There is also a much rarer form of pancreatic cancer which develops from islet cells in the pancreas and is known as pancreatic neuroendocrine cancer. Islet cells are responsible for secreting the hormone insulin which is required to regulate blood sugar, but these cancers are rare, comprising less than five percent of all cases of pancreatic cancer.
“Most of these neuroendocrine cancers are benign, but sometimes they can be aggressive,” says Prof Biankin. “For example, Steve Jobs died of pancreatic neuroendocrine cancer which had spread to his liver.”
What are the main risk factors?
Possible factors include:
Inherited gene mutations
Poor diet
Smoking and excessive alcohol consumption
Obesity
According to the American Cancer Society, around 10 per cent of cases of pancreatic cancer are thought to be directly linked to inherited gene mutations. For example, those with two or more first-degree relatives who have contracted the disease, have a greatly increased risk of developing it themselves.
However, because 80 per cent of pancreatic cancers occur in over-60s, the majority of cases are thought to stem from DNA damage accrued by various lifestyle factors over many years and decades. Earlier this year, a study in The Lancet found that people living in Western Europe are more likely to develop pancreatic cancer than anywhere else in the world, something which may be linked to excess alcohol intake, sedentary behaviour, red meat consumption and obesity.
Population studies have found that smokers are twice as likely to develop cancer, while regularly consuming excessive amounts of alcohol can lead to a condition called pancreatitis or inflammation of the pancreas, which can then develop into cancer.
“We don’t fully understand exactly what causes pancreatic cancer, but we do know some of the risk factors,” says Anna Jewell, the director of support, research and influencing at Pancreatic Cancer UK. “Things like age, smoking, being overweight and a recent diagnosis of diabetes may increase your risk. There are also other risk factors for which there is less evidence, for example eating high levels of red and processed meat.”
What are the symptoms?
One of the biggest problems when it comes to treating pancreatic cancer is that the disease is often symptomless in its early stages when it is still confined to the pancreas. Jewell says that typically patients only begin to realise that something is amiss, once tumours have grown and spread to other parts of the body.
People may begin to experience:
Back or tummy pain
Indigestion
Unexpected weight loss or changes to their poo
However, “these vague symptoms are common to many much less serious health conditions,” says Jewell, “and doctors face a significant challenge in deciding who to urgently refer for tests. If these symptoms persist for more than four weeks, they should be checked out.
Anyone experiencing the following should go straight to A&E, says Jewell:
Jaundice
Yellow eyes or skin
Itchy skin
How is pancreatic cancer diagnosed?
Blood and urine tests
CT scans or specialised endoscopy
Breath tests if available
Doctors currently diagnose the disease through blood and urine tests when patients present with tell-tale signs of jaundice or weight loss. If cancer is suspected, further investigations are carried out such as CT scans or a specialised endoscopy to examine the pancreas.
However, because jaundice and weight loss are signs of serious disease, 80 percent of pancreatic cancer patients end up being diagnosed at a very advanced stage when treatment options are limited.
As part of the push for early detection, Pancreatic Cancer UK are funding researchers at Imperial College London to try and develop the world’s first breath test which could be used by GPs as a low-cost, easy way of screening patients presenting with vague symptoms. This work is based on previous research which has shown that the presence of certain cancers releases a distinctive trace of chemicals called volatile organic compounds which travel around the bloodstream to the lungs before being breathed out. Imperial scientists are examining samples from several hundred people with and without pancreatic cancer to try and identify a unique signature of these chemicals linked to the disease.
“In future, simply blowing into a bag at the GP surgery could quickly open the way for an urgent scan, and for those that need it, the chance of potentially lifesaving treatment,” says Jewell.
New diagnostics and cancer tests
In recent years, academic researchers and biotechs have been attempting to develop so-called liquid biopsies which can pick up early signs of pancreatic cancer through detecting changes in the blood. The Avantect Pancreatic Cancer Test, developed by US company ClearNote Health, looks to identify signs of DNA alterations which indicate the onset of cancerous cell transformation. The company released a study last year showing that it could correctly identify people in the earliest stages of the disease with an accuracy of 68.3 per cent, and the test is already commercially available in several European countries, albeit not yet in the UK.
Dave Mullarkey, the chief executive of ClearNote Health, explains that the idea is for the test to be used in high-risk populations such as people with a family history of the cancer or those who have been diagnosed with Type 2 diabetes.
“Patients recently diagnosed with new onset Type 2 diabetes are encouraged to become more proactive about their health, including being vigilant for opportunities to participate in testing initiatives that may arise, aimed at early pancreatic cancer detection,” he says.
Doctors at the Royal Marsden are currently conducting early phase trials of their own liquid biopsy test which aims to detect tumour DNA in samples of a patient’s blood. “In the next three to four years, we hope that liquid biopsies will be used to potentially diagnose pancreatic cancer patients without the need for invasive tests,” says Bhogal.
Staging and grading of pancreatic cancer
The hope is that these diagnostics can ultimately lead to doctors regularly diagnosing patients at stage one or two when the disease is still confined to the pancreas. When patients are identified at stages three and four, this means that the cancer has already spread to other parts of the body and life expectancy is greatly reduced.
“We want to be able to identify patients at stage one or two because that’s ultimately where we can offer surgery,” says Bhogal. “This still remains the only real chance of a cure for pancreatic cancer. We can operate on some patients with more advanced disease but in these cases, the risks of the tumour coming back are greater.”
What is the life expectancy for pancreatic cancer?
Right now, the survival rates for pancreatic cancer are grim, with more than half of patients dying within three months of diagnosis and just 20 per cent still surviving at one year. According to the BMJ, pancreatic cancer survival rates in the UK are among the worst in Europe, with just 7 per cent of patients living for five years or longer. In comparison, five-year survival rates for breast cancer are 90 per cent.
Jewell believes that this bleak outlook is a consequence of decades of chronic underfunding, despite the disease being the deadliest common cancer. As a result, Pancreatic Cancer UK are now calling for cancer funding bodies to commit £35 million a year towards pancreatic cancer research to help accelerate much-needed breakthroughs in early diagnosis and treatments.
“This devastating disease has been neglected for decades,” she says. “It receives just 3 per cent of the UK cancer research budget and has too often been absent from national cancer strategies. We know that the right level of sustained funding can change everything. Survival rates for leukaemia have quadrupled thanks to significant and consistent investment in research.”
What treatments are emerging for pancreatic cancer?
In April 2024, scientists at UC San Francisco revealed they have developed the first small molecule drug capable of targeting a particular mutation, called G12D, which itself is responsible for nearly half of pancreatic cancer cases. This drug candidate is now hoped to enter clinical trials within the next two to three years.
Right now, the major shift in pancreatic cancer treatment is based around increasing the proportion of patients who can undergo surgery. According to Bhogal, only 25-30 per cent of patients are diagnosed at a stage where surgery is still possible, but if the pancreatic tumour is too large, an operation to remove it may be considered too dangerous.
Chemotherapy and radiotherapy
However, a series of trials around the world have shown that a combination of chemotherapy and radiotherapy treatment can be used to first shrink the tumour, allowing surgeons to then go in and take it out. “There’s patients who five, six years ago would not have been considered suitable for surgery, but are now falling in that pool,” says Bhogal.
Personalised approach
Oncologists are also looking to move towards a more personalised approach when deciding which chemotherapy to opt for, inspired by research done at Heidelberg University Hospital in Germany which has shown that conducting DNA sequencing on a patient’s tumour, can help reveal which drug it might be most sensitive to.
Bhogal says that this approach is currently being trialled in the UK, and if shown to be beneficial, such genetic-based approaches to selecting drugs could become part of the NHS care pathway in the next three to four years.
“For adenocarcinoma, there’s two chemotherapies we tend to use, called Folfirinox and gemcitabine,” he says. “Folfirinox works best in most patients but we’re learning that in some patients where the tumour has a particular molecular structure, it’s gemcitabine that works best.”
New therapeutics
There are also hopes that in the coming years, some completely new therapeutic approaches may begin to emerge for pancreatic cancer, although all are currently in early-stage trials. Prof Biankin says that Bristol Myers Squibb, Revolution Medicines and Astellas Pharma are all pursuing various ways of targeting KRAS proteins linked to pancreatic cancer. There are also hopes that messenger RNA (mRNA)-based cancer vaccines could also open up a new avenue for tackling the disease by training the immune system to recognise and kill pancreatic cancer cells.
In 2023, updated results from a phase one trial of a mRNA vaccine tested in 16 pancreatic cancer patients in combination with chemotherapy and immunotherapy found that within a year and a half of completing treatment, the cancer had not returned in half the participants.
How best can you live with pancreatic cancer?
One of the major challenges for people living with the disease is that the pancreas produces vital enzymes which the body needs to break down food and absorb nutrients. But as pancreatic cancers grow, they stop the production of these enzymes.
Jewell says that because of this, it is crucial for all patients to be prescribed pancreatic enzyme replacement therapy (PERT), tablets which help them live as well as possible with their illness, and ensure they remain strong enough to manage some of the debilitating symptoms and tolerate treatment.
“The disease will affect everyone differently,” says Jewell. “Some people may have vague symptoms around the point of diagnosis that may develop over time, whereas for others it may progress more rapidly.”
Ultimately the decisions which different patients take tend to be highly individual and depend on the stage of the cancer and personal choices.
“Chemotherapy may be suitable for some people while others may not be well enough to tolerate the side effects or choose not to have treatment,” says Jewell.
“Whatever people feel is right for them, it’s important that they receive support, including in accessing palliative care, to give them the best quality of life and as much precious time as possible with their loved ones.”
Pancreatic Cancer UK runs a dedicated Support Line for patients and their loved ones, staffed by specialist nurses. They provide expert, confidential, support and information. Freephone 0808 801 0707 or for more information visit: www.pancreaticcancer.org.uk/support


